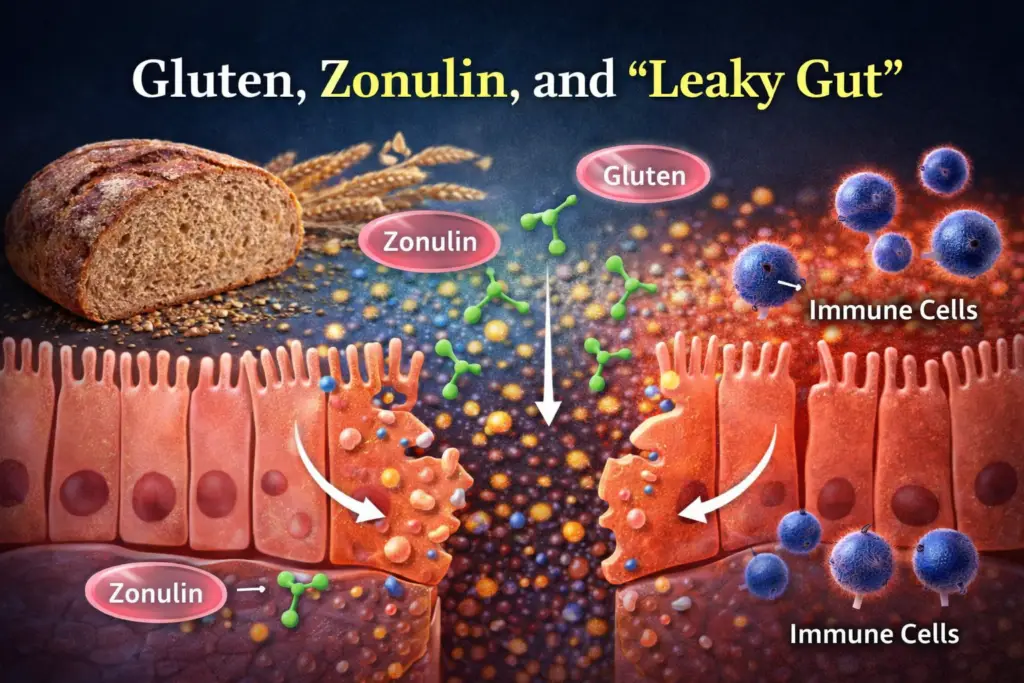
Gluten, Zonulin, and “Leaky Gut”
The Biological Mechanism Linking Gluten to Autoimmune Disease
In the previous articles in this series, “Gluten: What’s the Story” and “Why Some People Tolerate Gluten in Europe but Not in the United States”, we explored the idea that gluten-containing foods may trigger autoimmune responses in some people. If that is true, an important question follows: why does gluten trigger autoimmune disease in some individuals while others can eat wheat their entire lives without problems?
Another interesting question is whether tolerance can change over time. Can someone eat gluten without problems for decades and then suddenly find that it becomes less tolerable later in life?
When we ask these questions, it is important to remember that we are not dealing with a simple cause-and-effect relationship. Gluten is a complex molecule, and autoimmune disease is a complex biological process. This is not like the pain you feel after hitting your finger with a hammer.
Instead, the answer likely involves a complicated interaction between genetics, the immune system, the intestinal barrier, and the gut microbiome. Admittedly, these ideas are complex and still evolving. What follows is the current scientific understanding as I understand it today.
Over the past two decades, research has identified a key molecule—zonulin—that may help explain how gluten can trigger autoimmune disease in susceptible individuals.
The Gut Barrier: A Critical Defense System
The concept of “leaky gut” is controversial. Some physicians strongly support the idea of increased intestinal permeability, while others remain skeptical of how the concept is used outside scientific literature.
Setting the debate aside for a moment, it is useful to understand how the gut normally works.
The small intestine forms one of the most important protective barriers in the human body, along with the skin. The intestinal lining is made of epithelial cells connected by protein structures called tight junctions, which regulate what molecules can pass from the digestive tract into the bloodstream [1].
When functioning properly, this barrier allows nutrients to pass into the body while preventing bacteria, toxins, and large proteins from entering circulation.
However, if these tight junctions loosen, the intestinal barrier becomes more permeable. Scientists refer to this condition as increased intestinal permeability, sometimes referred to as “leaky gut.”
Research has linked increased intestinal permeability to several autoimmune diseases, including:
- celiac disease
- type 1 diabetes
- inflammatory bowel disease [2]
Zonulin: The Molecular Switch
In 2000, researchers identified zonulin, a protein that regulates tight junctions in the intestinal wall.
Zonulin acts as a biological signal that can temporarily open tight junctions, allowing molecules to pass through the intestinal barrier.
Under normal circumstances, this mechanism plays a role in regulating immune responses and intestinal function. However, excessive zonulin activity can lead to abnormal intestinal permeability.
The discovery of zonulin was made by gastroenterologist Dr. Alessio Fasano and colleagues. Fasano explained the significance of this finding:
“The zonulin pathway represents a potentially critical mechanism in the development of autoimmune diseases.” [3]
How Gluten Activates Zonulin
Research has shown that gliadin, one of the main proteins found in gluten, can activate the zonulin pathway.
Laboratory studies demonstrate that exposure to gliadin can trigger the release of zonulin from intestinal cells. This causes tight junctions to open and increases intestinal permeability [4].
When this occurs, larger molecules—including partially digested gluten peptides—can cross the intestinal barrier and interact with immune cells.
In individuals with genetic susceptibility, this immune activation may trigger the autoimmune cascade that defines celiac disease.
The Three Requirements for Autoimmune Disease
Dr. Fasano has proposed that three conditions must occur for autoimmune disease to develop:
- Genetic susceptibility
- An environmental trigger
- Loss of intestinal barrier function
In the case of celiac disease:
- the genetic susceptibility involves HLA-DQ2 or HLA-DQ8 genes
- the environmental trigger is gluten
- the barrier dysfunction occurs through zonulin-mediated permeability
Fasano summarized the theory clearly:
“Loss of intestinal barrier function appears to be a necessary step in the pathogenesis of autoimmune diseases.” [5]
The Microbiome Connection
Another critical factor in gluten tolerance is the gut microbiome.
It is estimated that the human body contains trillions of microorganisms living both inside and on the body. In fact, the number of microbial cells associated with the human body is roughly comparable to the number of human cells.
Sometimes I find it fascinating to think about this relationship. In many ways, we are ecosystems as much as we are individuals.
These microorganisms perform many important functions. For example, gut bacteria play a role in signaling intestinal cells to produce serotonin, a neurotransmitter that influences mood and other physiological processes.
Within the digestive system, microbes help regulate:
- digestion
- immune function
- intestinal barrier integrity
Certain bacteria are capable of breaking down gluten peptides, potentially reducing their immunogenic effects. Other microbial communities help maintain the intestinal barrier by regulating inflammation and tight junction proteins.
Conversely, microbiome imbalances—sometimes called dysbiosis—may increase intestinal permeability and immune activation [6].
Microbiome researcher Dr. Elena Verdu explains:
“The interaction between diet, the microbiome, and intestinal barrier function may determine whether gluten triggers inflammation or is tolerated normally.” [6]
Zonulin as a Biomarker
Scientists are now studying zonulin levels in blood and intestinal tissue as a possible biomarker of disease risk.
Elevated zonulin levels have been detected in individuals with:
- celiac disease
- type 1 diabetes
- inflammatory bowel disease [7]
Some research even suggests that increased zonulin levels may appear before the clinical onset of celiac disease, indicating that intestinal barrier dysfunction may precede autoimmune activation.
Implications for Autoimmune Disease
The zonulin pathway has implications far beyond gluten intolerance.
Researchers are currently exploring whether intestinal permeability may play a role in several autoimmune conditions, including:
- type 1 diabetes
- multiple sclerosis
- rheumatoid arthritis
- inflammatory bowel disease
Although research is ongoing, many scientists now believe that intestinal barrier dysfunction may be an important step in the development of autoimmune disease.
The Takeaway
Gluten does not cause autoimmune disease in most people. However, in genetically susceptible individuals, gluten may trigger a biological cascade involving:
- zonulin release
- increased intestinal permeability
- immune activation
- autoimmune inflammation
Understanding this pathway has changed how scientists think about both celiac disease and the broader relationship between diet, gut biology, and immune health.
As Dr. Fasano puts it:
“The intestine is not just a digestive organ—it is one of the most important regulators of the immune system.” [5]
Read the Other Articles in this Series
In this first article, “Gluten: What’s the Story?” I raised a few important questions and offer some ideas to think about.
In the second article, “Why Some People Tolerate Gluten in Europe but Not in the United States,” we will look at the science of gluten itself and explore possible explanations for why some people report different reactions depending on where they eat wheat products.
In the third article, “Gluten, Zonulin, and the ‘Leaky Gut’ Hypothesis: Why Gluten Triggers Autoimmune Disease in Some People,” we will look at a biological mechanism that may help explain why gluten causes inflammation in some individuals but not in others.
In the fourth article, “What Can Be Done to Reduce Zonulin and Support the Gut Barrier,” we will look at some practical recommendations for people who want to address some of the concerns raised in this series.
In the fifth article, “Gluten Sensitivity Test: How Do You Know If Gluten Is Affecting You?” we will look at how you can determine if you have a gluten sensitivity beyond celiac disease
References
- Turner, J. (2009). Intestinal mucosal barrier function in health and disease. Nature Reviews Immunology.
- Visser, J. et al. (2009). Tight junctions and autoimmune disease. Clinical Immunology.
- Fasano, A. (2000). Zonulin and intestinal permeability. Lancet.
- Lammers, K. et al. (2008). Gliadin induces zonulin release and increases intestinal permeability. Gastroenterology.
- Fasano, A. (2012). Leaky gut and autoimmune diseases. Clinical Reviews in Allergy and Immunology.
- Verdu, E. et al. (2015). The microbiome and gluten-related disorders. Gastroenterology.
- Sapone, A. et al. (2012). Zonulin and intestinal permeability in autoimmune diseases. Physiological Reviews.



Pingback: Gluten: What Is It Doing in the Body?